Reviewed by Jorge L. Flores, Esq. · Law Offices of Jorge L. Flores, P.A. · Miami, Florida · Last Updated: April 2026
Were You Just Told That an Earlier Scan Missed Something?
1. Write down today’s date and the date of the original scan. Florida law imposes a strict four year absolute deadline from the date the scan was performed. After that, your claim is permanently barred; even if you just found out about the error yesterday.
2. Request the original images immediately. Call the hospital or imaging center where the first scan was done. Ask for the actual images on a CD or digital transfer; not just the written report. You have a legal right to these under HIPAA and Florida Statute Section 456.057.
3. Request every scan taken since. The case is built by comparing the original “normal” scan against the later scan that revealed the problem.
4. Do not wait to “see how things go” with treatment. The legal deadline does not pause while you undergo chemotherapy, surgery, or rehabilitation. Contact an attorney before the deadline takes your case away.
The tumor was there. It was visible on the scan. The radiologist simply did not see it; or saw it and called it something else; or saw it, correctly identified it, and never told anyone. Eighteen months later, the cancer that was curable is now terminal. The image has not changed. The prognosis has.
The Law Offices of Jorge L. Flores, P.A., in Miami, Florida, understands that radiology malpractice occurs in the dark; the radiologist typically never meets the patient, the liability chain stretches across multiple corporate entities, and the catastrophic harm oftentimes does not surface until months or years after the original error. We are committed to providing aggressive, meticulous legal representation to patients and families throughout the State of Florida who have suffered devastating consequences because a medical image was misread, misinterpreted, or never communicated.
3-5%
Baseline Error Rate in Everyday Practice
~50%
Plaintiff Win Rate With Strong Evidence
51%
Minimum Survival Required Under Gooding
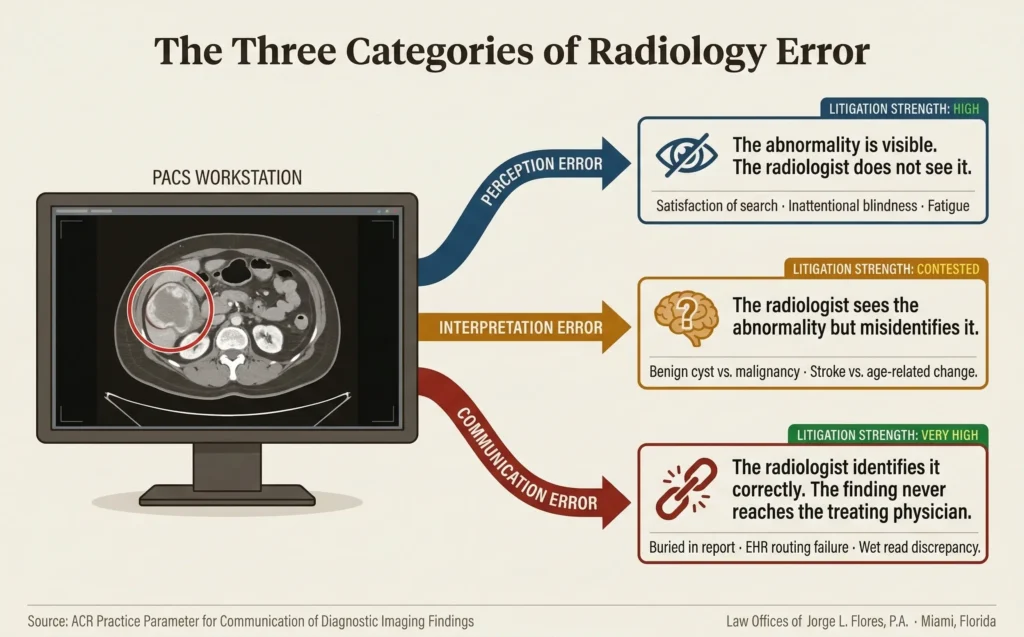
THE THREE CATEGORIES OF RADIOLOGY ERROR
Not every missed finding on a medical image constitutes medical negligence; radiology involves the probabilistic interpretation of complex anatomical shadows, and studies estimate a baseline error rate of 3% to 5% across everyday practice. However, when an error breaches the standard of care, it generally falls into one of three distinct categories.
|
Perception Error The abnormality is visibly present on the image, but the radiologist fails to detect it. Driven by “satisfaction of search” (finding one abnormality and stopping), inattentional blindness, fatigue from high reading volumes, and failure to compare with prior studies. These cases are oftentimes the strongest in litigation because the image is permanent, objective evidence. |
Interpretation Error The radiologist sees the abnormality but attributes it to the wrong clinical cause; classifying a malignant mass as a benign cyst, misreading an acute stroke as age related white matter change, or mischaracterizing severe spinal cord compression as mild disc disease. Defense will argue “reasonable judgment call.” |
Communication Error The radiologist perceives the abnormality, correctly identifies it as life threatening in the report; but the finding never reaches the treating physician. Critical results buried in lengthy reports, EHR routing failures, and “wet read” discrepancies. Juries respond with high verdicts because the radiologist’s own report proves they saw it. |
What This Means for Patients
The image is permanent. It does not change after it is taken. If a tumor, a blood clot, or a fracture was visible on a scan that was reported as “normal,” a subsequent expert can review the exact same image and identify what was missed. Unlike most medical malpractice cases where the evidence depends on clinical notes and witness testimony, in radiology cases the evidence is literally frozen in the picture.
WHO IS LIABLE FOR A RADIOLOGY ERROR IN FLORIDA
Radiology malpractice cases rarely involve a single defendant, because the diagnostic process relies on a chain of custody stretching from the ordering of the scan, to the acquisition of the images, to the interpretation, to the clinical follow up.
| Defendant | Basis of Liability |
|---|---|
| Interpreting Radiologist | Primary individual liability for perception and interpretation errors. Held to the specialist standard under Section 766.102; measured against what reasonably prudent radiologists in the same subspecialty would recognize as acceptable. |
| Referring / Treating Physician | Independent, non delegable duty to obtain results, review them, and act upon them. If the radiologist’s report accurately identifies a tumor but the referring physician fails to act, primary liability shifts. EHR audit trails prove exactly when the report was opened and by whom. |
| Hospital / Imaging Center | Vicariously liable if the radiologist is a direct employee. If the radiologist is an independent contractor, the hospital may still be liable under the doctrine of apparent agency. Also directly liable under Section 766.110 for outdated equipment, dangerous staffing levels causing radiologist fatigue, or failure to implement reliable critical result communication systems. |
| Radiology Technologist | Liable if poor patient positioning, motion artifact, improper contrast use, or wrong imaging sequences prevented a proper interpretation. Also has a professional duty to flag obvious emergent findings to the radiologist. |
| Teleradiologist (Out of State) | Under Florida Administrative Code Rule 64B8-9.010, any radiologist providing a primary interpretation relied upon for treating a Florida patient is practicing medicine in Florida and must hold a valid Florida license. If unlicensed, the referring Florida physician retains primary responsibility. |
If you believe an imaging study was misread and the delay caused your condition to worsen, contact the Law Offices of Jorge L. Flores, P.A. for a free consultation.
THE MOST DANGEROUS MISSES BY IMAGING TYPE
| Imaging Modality | Common Missed Findings | Why It Matters in Litigation |
|---|---|---|
| Mammography | Breast cancer masses, microcalcifications, architectural distortion, asymmetric density | Highest value malpractice area due to delayed cancer staging. Dense breast tissue masks tumors. Florida Statute Section 381.933 mandates facilities notify patients of dense breast tissue. |
| CT Scan | Strokes, pulmonary embolisms, appendicitis, aortic aneurysms, incidental cancerous nodules | Primary ER imaging tool; highly susceptible to perception errors from fatigue and volume. Missed stroke or PE leads to catastrophic brain damage or sudden death. |
| MRI | Spinal cord compression, brain tumors, acute strokes, severe tendon tears | Complex pulse sequences requiring subspecialty expertise. Delays in diagnosing spinal cord compression cause irreversible ischemia and permanent paralysis. |
| Ultrasound | Ectopic pregnancies, testicular/ovarian carcinomas, deep vein thrombosis, gallbladder pathology | Highly operator dependent. Frequent “error of omission”; failing to order the scan when clinically indicated. Missed ectopic pregnancy causes fatal hemorrhaging. |
| X Ray | Early lung cancer nodules, subtle fractures (scaphoid, cervical spine), pneumonia | Three dimensional anatomy compressed into two dimensions. Early lung nodules visible on routine chest X ray are missed, allowing progression to Stage IV. |
| PET Scan | Cancer staging errors; under staging or over staging malignancies | Requires exact correlation with structural imaging. Errors occur when PET is read in isolation or abnormal metabolic uptake is incorrectly attributed to infection rather than metastasis. |
THE 51 PERCENT RULE AND DELAYED DIAGNOSIS
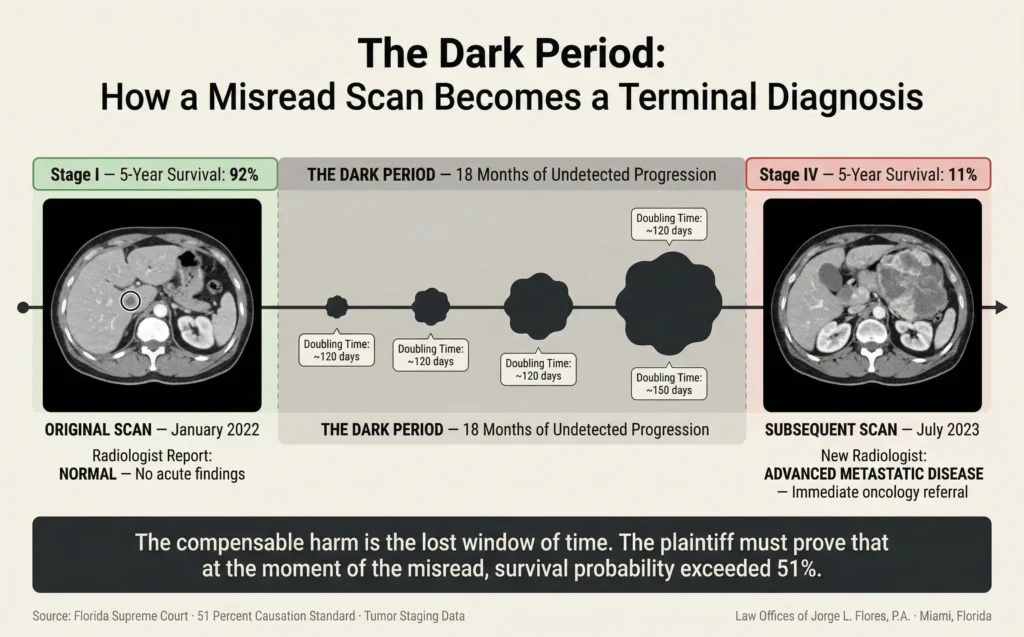
A misread scan does not create the patient’s tumor; the tumor was already growing. The harm caused by the radiologist is the delay in diagnosis and the unchecked progression of the underlying disease.
Florida Rejects “Loss of Chance”
If a patient had a 49% chance of survival when the scan was misread, and the delay reduced that chance to 0%, the patient has no legal cause of action in Florida. The plaintiff must prove it is more likely than not; meaning a greater than 50% probability; that the injury or death would have been avoided but for the radiologist’s specific negligence. See our misdiagnosis guide for the full analysis of the Gooding standard.
How We Prove Causation
In cancer cases, we deploy the “staging argument”; proving the cancer was at a curable stage on the date the scan was misread and advanced to an incurable stage during the delay. In stroke cases, we invoke “time is brain”; proving the treatment window closed because of the misread. We use tumor doubling time calculations, historical survival data, and precise medical staging to cross the 51% threshold.
The Statute of Repose; The Hidden Deadline That Kills Radiology Claims
It is significant to note that while Florida’s Discovery Rule allows the two year limitation clock to begin when the patient discovers the misread, an absolute four year Statute of Repose bars all claims filed more than four years after the negligent act, regardless of when the error was finally discovered. If a radiologist misses a tumor on an MRI in January 2022 and the patient does not learn of the error until February 2026, the case is permanently barred. Filing a Notice of Intent before the repose period expires will toll the deadline, as confirmed in Musculoskeletal Inst. Chartered v. Parham. For the full pre suit process, see our pre suit requirements guide.
FLORIDA RADIOLOGY VERDICTS AND SETTLEMENTS
| Amount | Jurisdiction | What Happened |
|---|---|---|
| $217 Million | Hillsborough County | 50 year old man presented with clear stroke symptoms; incorrectly discharged with a sinusitis diagnosis. Catastrophic brain swelling the next day. Permanently wheelchair bound, brain damaged. Jury awarded $116.7M compensatory + $100.1M punitive. |
| $21.6 Million | Miami Dade County | 47 year old nurse had a cancerous breast lump continuously misdiagnosed as mastitis over an entire year. Multiple ultrasounds and a mammogram misinterpreted. Cancer advanced to incurable stage. |
| $7 Million | Florida (Settlement) | Post operative MRI ordered for spinal cord compression. Failures in timely diagnosis based on imaging led to permanent loss of motor function in both legs. |
| $2 Million | Florida (Settlement) | Emergency providers and radiologists failed to properly diagnose a pulmonary embolism on diagnostic imaging. Fatal cardiac event followed. |
The Four Year Wall Is the Biggest Threat to Radiology Claims
In most malpractice cases, you have two years from the date you discover the error. But Florida’s four year statute of repose is an absolute wall; it runs from the date the scan was performed, not the date you found out about the mistake. If a radiologist misreads your scan today and you do not learn about it for three years and eleven months, you have one month to file. If you learn about it at four years and one day, your case is permanently dead. This is why radiology claims require immediate legal consultation the moment a new provider tells you an earlier scan missed something.
Inside Advantage
The defense in a radiology case never concedes the miss. They retain their own board certified radiologist who reviews the same image and testifies that the finding was “subtle,” “equivocal,” or “within the range of normal variation.” Before founding this firm, Attorney Flores defended these exact cases from the hospital side. He knows how defense radiology experts are selected, how they frame their testimony around “retrospective bias,” and which specific visual characteristics of the image they will emphasize to minimize the visibility of the missed finding. We build every radiology case by anticipating that defense narrative and systematically dismantling it before trial.
If you or a loved one has suffered a delayed cancer diagnosis, a missed stroke, or permanent disability because an imaging study was misread in Florida, the experienced Law Offices of Jorge L. Flores, P.A., can help.
From our offices in Miami, Florida, we obtain the original diagnostic images and every subsequent scan, retain independent board certified radiologists in the exact subspecialty, map the complete chain of custody through EHR audit trails, and build the staging and causation timeline necessary to cross the 51% threshold. We advance all costs of the investigation on your behalf. You pay nothing unless we recover compensation.
P.S. The image has not changed. It shows exactly what it showed on the day it was taken. If an abnormality that is now causing you catastrophic harm was visible on an earlier scan that was reported as normal, every day you wait moves you closer to the four year Statute of Repose; the absolute deadline after which Florida law permanently bars your claim regardless of when you discovered the error. Call the Law Offices of Jorge L. Flores, P.A., today; because the evidence is already preserved inside the image, and we know exactly how to extract it.
Related: Medical Malpractice · Misdiagnosis · Delayed Diagnosis · ER Misdiagnosis · Brain and Spinal Cord Injuries