Reviewed by Jorge L. Flores, Esq. · Law Offices of Jorge L. Flores, P.A. · Miami, Florida · Last Updated: April 2026
You described your symptoms through a screen. The doctor could not touch you, could not listen to your heart, could not press on your abdomen to check for the rebound tenderness that would have revealed the emergency. They told you it was probably nothing. Hours later, you were in an ambulance.
The Law Offices of Jorge L. Flores, P.A., in Miami, Florida, understands that telehealth malpractice represents one of the most rapidly emerging and uniquely complex frontiers of medical malpractice in the State of Florida. Approximately 62% of Florida residents have utilized telehealth services, and for many; particularly rural populations, elderly individuals, and those with limited access to in person care; virtual medicine has shifted from a pandemic era workaround to a primary access point for medical assessment. While diagnostic errors account for 40% to 50% of traditional malpractice claims, misdiagnosis is the primary factor in 66% to 70% of telehealth malpractice claims.
IF A TELEHEALTH VISIT LED TO A MISSED EMERGENCY
Telehealth evidence lives on app servers that platforms can purge after retention periods expire. Screenshot the app showing the appointment date, time, duration, and the provider’s name. Download every chat message, secure message, and intake questionnaire you submitted through the portal. Save the after visit summary, any digital prescriptions, and all email confirmations. If the platform told you the visit was being recorded, send a written request for a copy of that video file today. Write down exactly what symptoms you described on camera, what the provider said in response, and whether the video or audio was lagging. Search the Florida Department of Health license verification portal to confirm the provider holds a valid Florida license. Contact an attorney so we can subpoena the platform’s backend data before it is deleted.
66-70%
Of Telehealth Claims Involve Misdiagnosis
62%
Of Floridians Have Used Telehealth
$36M
Cerebral DEA/DOJ Settlement
THE SAME STANDARD OF CARE; WITH LESS INFORMATION
The foundational provision of the Florida Telehealth Act, codified in Section 456.47 of the Florida Statutes, creates a profound clinical paradox. The statute declares that a telehealth provider has the duty to practice in a manner consistent with the prevailing professional standard of practice for a healthcare professional who provides in person healthcare services. Florida law affords no “telehealth discount” on clinical quality. A physician diagnosing a patient over a webcam is held to the exact same standard as if the patient were sitting in a physical examination room; yet the provider possesses significantly less diagnostic information.
Florida Statute Section 456.47; The Telehealth Act
If an in person standard of care for a specific presentation requires palpation, auscultation, or an immediate diagnostic test such as an EKG or CT scan, the telehealth provider must direct the patient to a facility where those assessments can occur. Attempting to guess the diagnosis virtually when the clinical presentation demands a physical examination constitutes a breach of duty under Florida law.
What This Means for Patients
Your virtual doctor was legally required to give you the same quality of care as if you were sitting in their office. If they could not figure out what was wrong without touching you, they were supposed to send you to someone who could. If they guessed instead, that is where the malpractice begins.
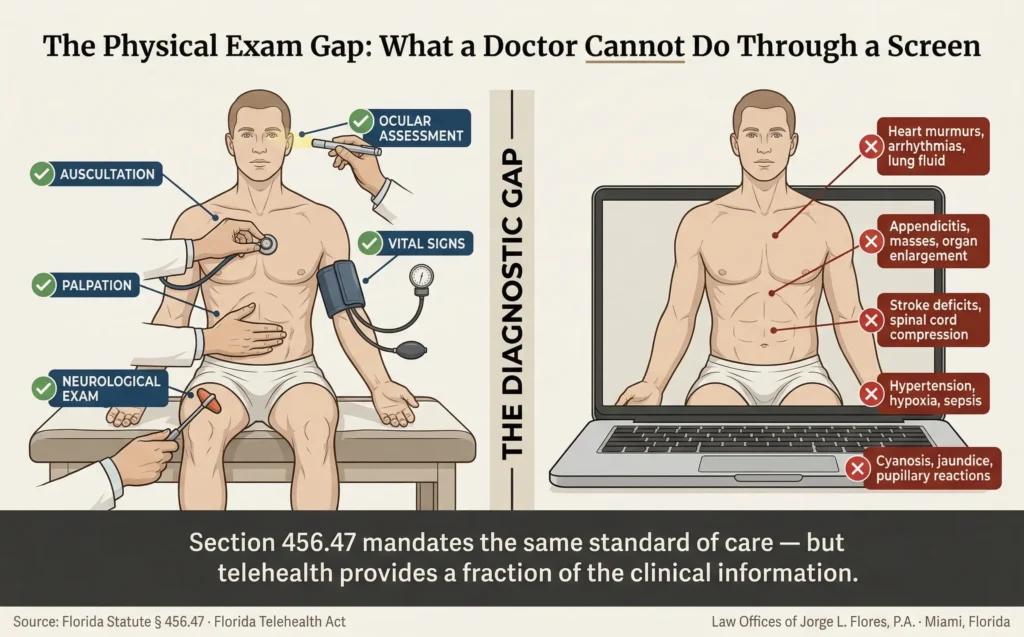
WHAT A DOCTOR CANNOT DO THROUGH A SCREEN
| Clinical Assessment | In Person | Telehealth Limitation | What Gets Missed |
|---|---|---|---|
| Auscultation | Stethoscope on the chest, abdomen, and neck | Impossible without patient owned Bluetooth devices | Heart murmurs, arrhythmias, fluid in the lungs, absent bowel sounds |
| Palpation | Hands pressing on the body | Completely impossible | Rebound tenderness (appendicitis), hidden masses, abnormal pulses |
| Neurological Exam | Deep tendon reflexes, muscle strength, sensory assessment | Severely limited to crude visual observation | Focal deficits indicating stroke or spinal cord compression |
| Vital Signs | Calibrated BP cuff, pulse oximeter, clinical thermometer | Patient reported data from uncalibrated home devices | Hypertensive crisis, hypoxia, systemic sepsis |
| Skin / Ocular | Direct observation under clinical lighting | Degraded by video resolution, poor lighting | Cyanosis, jaundice, pupillary reactions |
If a telehealth provider failed to refer you to emergency care and your condition worsened, contact the Law Offices of Jorge L. Flores, P.A. for a free consultation.
THE MALPRACTICE SCENARIOS WE LITIGATE
|
Misdiagnosis From the Physical Exam Gap Chest pain diagnosed as anxiety because the provider could not perform an EKG. Abdominal pain dismissed as gastroenteritis because the provider could not palpate for rebound tenderness. The provider’s failure to recognize that these symptoms cannot be ruled out virtually is the breach. |
Failure to Triage and Refer Patient describes the “worst headache of their life,” sudden unilateral weakness, or severe shortness of breath. Instead of directing the patient to call 911, the provider offers false reassurance or advises rest. The delay in emergent intervention results in permanent brain injury, paralysis, or death. |
Dangerous Virtual Prescribing Powerful medications authorized after a cursory five minute video chat without verifying weight, vitals, or current drug regimen. Corporate platforms incentivizing rapid prescribing of Schedule II controlled substances in violation of Section 456.47(2)(c). |
Schedule II Controlled Substance Restrictions; Section 456.47(2)(c)
Florida law strictly prohibits telehealth providers from prescribing Schedule II controlled substances via virtual visit, with only four narrow exceptions: treatment of psychiatric disorders, inpatient hospital care, hospice services, and nursing home residents. Violations form the foundation for “negligence per se” arguments.
WHO CAN BE SUED FOR TELEHEALTH MALPRACTICE
Identifying the correct defendants requires unraveling corporate structures specifically designed to shield billion dollar platforms from liability.
| Defendant | Theory of Liability |
|---|---|
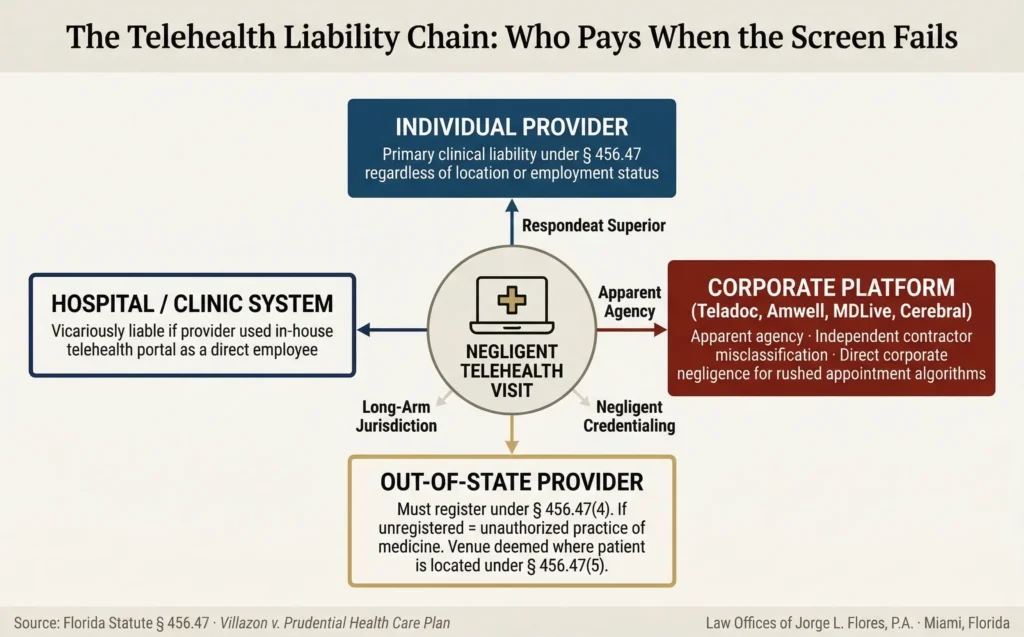
| Individual Provider | The physician, APRN, or PA who conducted the virtual encounter retains ultimate responsibility under Section 456.47. |
| Telehealth Platform | Platforms classify doctors as “1099 independent contractors” to avoid liability. We pierce this through independent contractor misclassification, apparent agency, and direct corporate negligence (dangerously rushed appointment times, failure to credential providers). |
| Hospital or Clinic System | If the virtual visit was conducted by a provider employed by a Florida hospital using its own telehealth portal, the hospital is vicariously liable. |
| Out of State Provider | Under Section 456.47(4), any out of state provider treating a Florida patient must register with the Florida Department of Health. If unregistered, they may have engaged in the unauthorized practice of medicine. Section 456.47(5) establishes that telehealth services are legally deemed to occur where the patient is located. |
The Bottom Line for Patients
You do not just sue the individual doctor who was on the screen. The company behind the app; Teladoc, Amwell, BetterHelp, Cerebral, or whoever owns the platform; can also be held responsible, especially if they controlled how the doctor practiced, how long the visit lasted, or failed to check whether the doctor was even properly licensed.
THE DIGITAL EVIDENCE THAT WINS THESE CASES
|
Connection Logs Timestamps showing when the provider joined, when they disconnected, and the total duration. A log proving a complex diagnostic visit lasted 90 seconds is powerful objective evidence of a rushed, negligent assessment. |
EHR Audit Trails Metadata revealing when the provider accessed the patient’s chart, what documents they viewed, and whether they ignored critical system alerts regarding drug interactions or abnormal lab results. |
Visit Recordings Florida is a strict two party consent state under Section 934.03. However, if the platform recorded the session with consent for “quality assurance,” that video is highly discoverable and serves as the cornerstone of the case. |
Inside Advantage
Telehealth platforms do not defend these cases by conceding the misdiagnosis. They make the patient disappear behind layers of corporate architecture. Before founding this firm, Attorney Flores spent years on the defense side of medical malpractice litigation in Miami and understands exactly how corporate defendants layer these arguments. We dismantle that architecture one layer at a time; subpoenaing the platform’s backend connection logs, deposing corporate officers on appointment length algorithms, and running the independent contractor misclassification analysis that restores vicarious liability to the billion dollar company that profited from the visit.
Telehealth malpractice claims are subject to the same Chapter 766 pre suit requirements as traditional malpractice cases. For the types of damages and fee structure, see the linked guides.
If you or a loved one has suffered catastrophic harm because a telehealth provider failed to recognize an emergency, prescribed a dangerous medication without adequate evaluation, or refused to refer you to in person care, the experienced Law Offices of Jorge L. Flores, P.A., can help.
From our offices in Miami, Florida, we subpoena platform connection logs, EHR audit trails, and corporate appointment length algorithms. We advance all costs. You pay nothing unless we recover compensation.
P.S. The telehealth platform’s connection log still exists. It shows exactly how long your visit lasted, what time the provider joined and disconnected, and whether the encounter was long enough to constitute a competent clinical assessment. That metadata does not lie, and it does not change. But platforms routinely purge data after retention periods expire. Call the Law Offices of Jorge L. Flores, P.A., today; before the digital evidence that proves your case is deleted.
Related: Medical Malpractice · Misdiagnosis · Medication Errors · ER Misdiagnosis · Who Can Be Held Responsible


