Reviewed by Jorge L. Flores, Esq. · Law Offices of Jorge L. Flores, P.A. · Miami, Florida · Last Updated: April 2026
“Why did no one tell me this could happen?” When a known but undisclosed surgical risk materializes; leaving a patient with permanent nerve damage, disfigurement, or catastrophic disability; the failure is not merely a bad outcome. It is a violation of the patient’s fundamental right to make an informed decision about their own body.
The Law Offices of Jorge L. Flores, P.A., in Miami, Florida, understands that informed consent litigation is one of the most widely misunderstood and uniquely challenging areas of medical malpractice law in the State of Florida. A prevalent assumption among patients is that a physician’s failure to verbalize a specific risk automatically constitutes grounds for a successful lawsuit. A prevalent assumption among healthcare providers is that a patient’s signature on a standardized hospital consent form provides absolute legal immunity. Under Florida law, both of these assumptions are fundamentally incorrect.
IF YOU SUFFERED A COMPLICATION YOUR DOCTOR NEVER WARNED YOU ABOUT
Request your complete medical records immediately; demand the signed consent forms, the physician’s pre operative clinical notes, the surgical operative report, and the minute by minute nursing flowsheets from the day of the procedure. Preserve the physical consent form itself. We scrutinize this document not to confirm a signature, but to assess whether it consisted of vague boilerplate language or specifically enumerated the catastrophic complication that actually occurred. Write down every detail you recall about the pre operative consultation; what the doctor explicitly said, what questions were asked, the duration of the conversation, and whether you were already sedated at the time. Do not assume the signed form protects the hospital. Under Florida law, a signature creates only a “rebuttable presumption” of valid consent; it is a piece of evidence, not an ironclad shield. Contact an attorney before memories fade and statutory clocks expire.
WHAT INFORMED CONSENT REQUIRES UNDER FLORIDA LAW
Florida Statute Section 766.103, formally known as the Florida Medical Consent Law, dictates that a medical provider must ensure the patient gains a “general understanding” of three specific elements before any non emergency medical intervention is performed.
Disclosure 01 — The Nature of the Procedure
What the medical intervention entails, the physical actions the surgeon will take, and the intended anatomical or physiological purpose of the treatment.
Disclosure 02 — Substantial Risks and Hazards
The known, significant dangers inherent in the proposed treatment. Florida courts evaluate “substantial” by weighing the statistical probability of the complication against the severity of the potential harm; a rare but catastrophic risk such as permanent paralysis may require disclosure just as much as a minor but highly likely complication.
Disclosure 03 — Reasonable Alternatives
Medically acceptable alternative procedures or treatments; crucially including the explicit option of doing nothing at all and the likely prognosis of that choice.
WHY A SIGNED CONSENT FORM DOES NOT PROTECT THE HOSPITAL
Under Section 766.103(4)(a), a validly signed consent form creates only a “rebuttable presumption” of valid consent. The Florida Supreme Court ruled in Parikh v. Cunningham (1986) that a signature alone does not grant immunity. Before any presumption of validity attaches, the trier of fact must determine that the substantive requirements of the consent law were met.
MYTH
“I signed the consent form, so there is nothing I can do. The hospital is protected.”
REALITY
The presumption is rebutted if the form was signed under sedation, if the physician misrepresented or concealed a known risk (Public Health Trust v. Valcin, 1987), or if the form used generic boilerplate language that failed to specify the actual substantial risks of the exact procedure.
What This Means for Patients
A signed consent form is not the end of the conversation. It is the beginning. If your doctor handed you a clipboard with generic language about “infection, bleeding, and death” but never told you that the specific procedure carried a known risk of permanent nerve damage; and that is exactly what happened to you; the form does not protect them. The question is not whether you signed. The question is whether the doctor actually explained the specific risk that materialized.
If you believe a physician failed to disclose the risks of a procedure before you consented, contact the Law Offices of Jorge L. Flores, P.A. for a free consultation.
THE DOUBLE TEST THAT MAKES THESE CASES UNIQUELY DIFFICULT
Winning a claim based solely on a lack of informed consent is notoriously difficult in Florida due to a unique “double test” embedded within Section 766.103.
Part 1: Standard of Practice Test
Under Section 766.103(3)(a)(1), a physician is protected if the disclosure was “in accordance with an accepted standard of medical practice among members of the medical profession with similar training and experience.” The plaintiff must retain an expert in the exact same specialty to testify the defendant deviated from the profession’s accepted disclosure norms.
Part 2: The “Would Have Consented Anyway” Test
Even if the plaintiff proves the physician blatantly failed Part 1, the case collapses under Section 766.103(3)(b) if a jury determines that a “reasonable person” facing the same medical circumstances would have proceeded with the treatment regardless. This objective standard; not the plaintiff’s subjective hindsight; is the definitive case killer in Florida informed consent litigation.
THE VALCIN DOCTRINE: SHIFTING THE BURDEN OF PROOF
In the landmark 1987 decision Public Health Trust of Dade County v. Valcin, the Florida Supreme Court established that when a healthcare provider fails to maintain necessary medical records, or when a patient provides evidence of fraudulent misrepresentation, a rebuttable presumption of negligence arises and the burden shifts to the provider.
What This Means for Your Case
While the Valcin burden shifting doctrine forces the defense onto their back foot, it does not bypass the “would have consented anyway” test. This is precisely why we never rely on a single legal theory; we build every informed consent case to withstand both halves of the double test.
CODE 15 REPORTS: THE SMOKING GUN
Under Section 395.0197 of the Florida Statutes, licensed medical facilities are mandated to file a “Code 15” adverse incident report with the Agency for Health Care Administration within 15 days if a patient requires surgical repair of damage resulting from a planned procedure; provided the damage was not a recognized specific risk disclosed to the patient.
Why This Matters
If a hospital files an AHCA Code 15 report regarding a surgical complication, it functions as a tacit institutional admission that the specific risk which materialized was definitively not disclosed to the patient beforehand. This is oftentimes the single most compelling piece of evidence a plaintiff can acquire in an informed consent case, and we aggressively pursue the production of these reports in every case we evaluate.
INFORMED CONSENT VS. MEDICAL BATTERY
Lack of Informed Consent (Negligence)
The patient authorized a specific procedure, but the physician negligently failed to adequately explain the risks. Subject to the full double test. Requires expert witness testimony.
Medical Battery (Intentional Tort)
The physician performed an entirely unauthorized, unconsented procedure; such as amputating the wrong limb or operating on the wrong organ. Does not require the “would have consented anyway” analysis. Does not strictly require expert testimony. Significantly easier to litigate.
Under Florida Administrative Code 64B8-9.007, the responsibility for obtaining informed consent is a strictly non delegable duty resting entirely upon the operating physician. The Florida Third District Court of Appeal reinforced this in Cedars Medical Center v. Ravelo (1999), ruling that liability belongs exclusively to the physician performing the procedure; not the hospital facility where the surgery took place. For the full analysis of who can be held responsible in a Florida malpractice case, see our liability guide.
WHEN INFORMED CONSENT CLAIMS SUCCEED AND WHEN THEY FAIL
| Scenario | Why It Succeeds or Fails | Strength |
|---|---|---|
| Elective cosmetic procedure; undisclosed risk of permanent nerve paralysis | Because the procedure was medically unnecessary, a jury is highly likely to believe a reasonable person would have declined. The “would have consented anyway” defense is exceptionally weak. | STRONG |
| Alternative treatment withheld; physician recommends invasive spinal fusion without disclosing physical therapy option | Failure to disclose “medically acceptable alternative procedures” as mandated by Section 766.103. | STRONG |
| Wrong procedure performed; patient consents to left toe amputation, team amputates the right | Transcends informed consent into medical battery. Does not require the double test. | VERY STRONG |
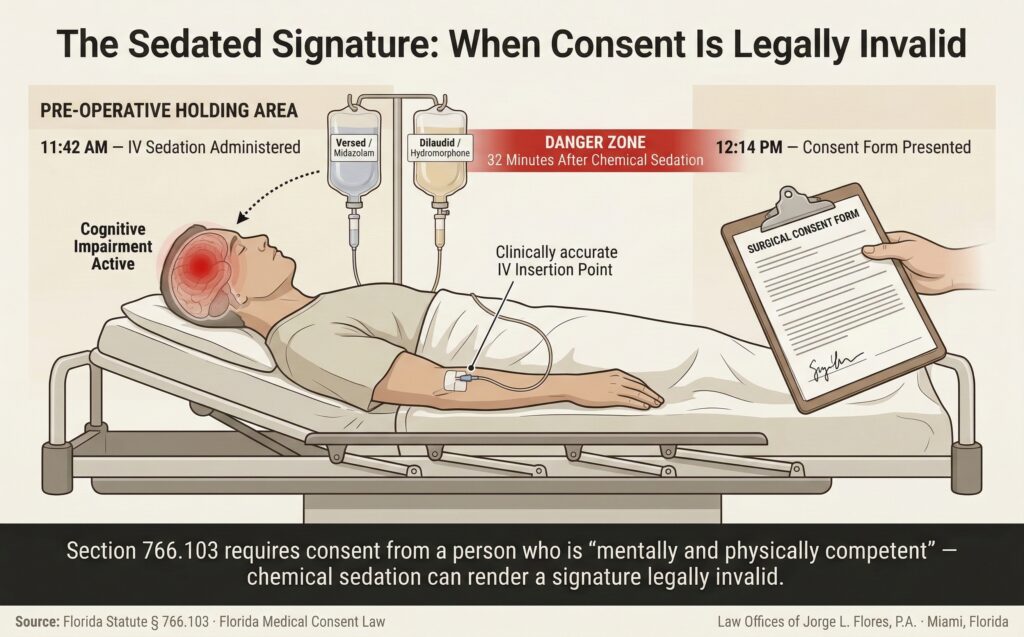
| Sedated signature; patient signs after heavy IV narcotics | Section 766.103 requires mental and physical competency. | MODERATE STRONG |
| Life saving emergency; surgeon fails to mention 5% risk before repairing ruptured aortic aneurysm | The “would have consented anyway” test destroys this claim. Emergency exceptions also apply. | WEAK |
| Properly disclosed bad outcome; risk was explained, patient consented, complication occurred | No viable claim. The patient assumed a known, disclosed risk. | NOT ACTIONABLE |
The Strongest Claims and the Weakest
Informed consent claims are strongest when the procedure was elective (the patient did not need it), when a safer alternative existed (the patient had a real choice), or when the doctor performed an entirely different procedure than what was authorized (medical battery). They are weakest when the procedure was life saving, because a jury will almost always conclude that a reasonable person would have accepted the risk rather than die. If your case involves an elective procedure with an undisclosed catastrophic risk, you have the strongest possible foundation for a claim.
This is why the Law Offices of Jorge L. Flores, P.A., builds the most powerful claims by pleading both a lack of informed consent and standard surgical negligence simultaneously; providing the jury with two distinct, independent pathways to reach a liability verdict. For the pre suit requirements, the types of damages, and how we get paid, see the linked guides.
Inside Advantage
Attorney Flores worked as an attorney for a top rated insurance defense firm in Miami, where he learned first hand how defense counsel deploys the “would have consented anyway” argument. He builds every case with a dual theory approach specifically designed to survive that defense; because we do not simply argue that the doctor failed to communicate. We simultaneously prove that the doctor failed to perform.
If you or a loved one has suffered catastrophic harm from an undisclosed surgical risk, the experienced Law Offices of Jorge L. Flores, P.A., can help you determine whether you have a viable informed consent claim, a medical battery action, or a dual theory negligence lawsuit.
From our offices in Miami, Florida, we retain same specialty medical experts, forensically analyze consent documents and Code 15 adverse incident reports, and build every case with the dual theory approach necessary to survive Florida’s uniquely challenging double test. We advance all costs. You pay nothing unless we recover compensation.
P.S. Not all bad outcomes are the result of medical errors or malpractice. However, if a physician withheld information about a substantial risk or a safer alternative, and that undisclosed risk is precisely what caused your catastrophic injury, the Law Offices of Jorge L. Flores, P.A., possesses the forensic expertise and the inside knowledge of defense strategy to determine whether you have a viable case. Call today; because you deserve an honest answer.
Related: Medical Malpractice · Surgical Errors · Anesthesia Errors · Birth Injuries · Pre Suit Requirements


