Written by Jorge L. Flores, Esq. · Law Offices of Jorge L. Flores, P.A. · Miami, Florida · Last Updated: March 2026
The surgeon says what happened was “just a complication.” The hospital calls it an “inherent risk.” They point to the consent form you signed. But the recovery was supposed to take three days, and you have been in the ICU for two weeks. You need to know whether this was bad luck or bad medicine.
That question is the legal boundary that determines everything. The Law Offices of Jorge L. Flores, P.A., in Miami, Florida, has built an entire practice around answering it; because the medical establishment routinely deploys the word “complication” as a catch all to obscure instances where substandard care directly caused the injury.
RED FLAGS THAT SUGGEST NEGLIGENCE, NOT A COMPLICATION
If any of the following happened to you, the “complication” defense may not hold.
A doctor at a different hospital said “this should not have happened” or expressed visible concern about the care you received. Hospital staff suddenly became evasive, refused to answer questions, or stopped visiting your room after the event. The hospital offered to waive your bills or asked you to sign a release before you understood the full extent of your injury. Your recovery was dramatically longer or more severe than the surgeon originally described. A nurse privately told you to “get a copy of your chart” or “talk to a lawyer.” The medical records contradict what you were told verbally; or there are gaps in vital sign monitoring during the period when your condition worsened. Standard prevention protocols were skipped: no compression boots, no blood thinners, no prophylactic antibiotics when they were required. Contact an attorney before the medical record is amended.
THREE QUESTIONS THAT DECIDE YOUR CASE
Under Florida Statute Section 766.102, the distinction between a complication and negligence is not defined by the injury itself. A blood clot, an infection, nerve damage; every one of these can be unavoidable biology or preventable malpractice.

Question 1: Did the doctor follow the accepted standard of care?
If the provider deviated from established surgical protocols, omitted mandatory prophylactic measures, or exhibited poor technique, the resulting harm is likely negligence.
Question 2: Once the problem appeared, was it caught and managed in time?
This is where most cases actually live. An unpreventable bowel perforation during a colonoscopy may be a known complication. Discharging the patient while they exhibit classic signs of peritonitis is not. The complication is not the malpractice; the failure to respond to it is.
Question 3: Were you told about this specific risk before you consented?
If a material risk was withheld, an informed consent claim may exist even if the procedure was technically perfect. You never consent to substandard care.
FIND YOUR SCENARIO
The same injury can go either way depending on what the doctor did. Each scenario is analyzed twice; once as a legitimate complication, once as actionable negligence.
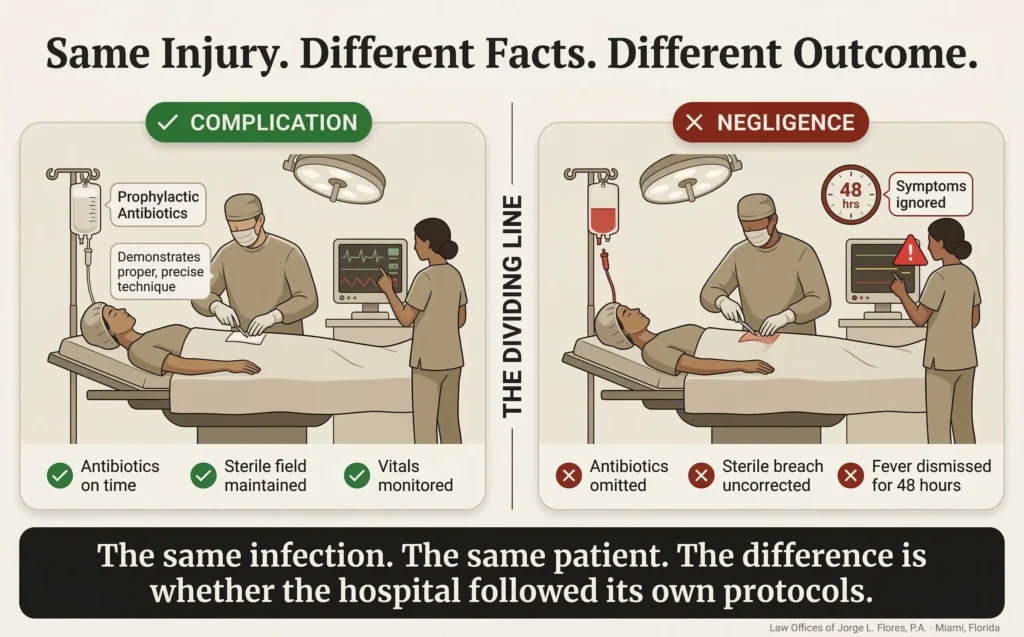
Surgical Site Infection
Complication
Antibiotics administered within the mandated 60 minute window. Sterile field maintained. Wound closed properly. Patient monitored. Infection developed anyway from the patient’s own biology; a statistical reality for 3% to 15% of surgical patients.
Negligence
Antibiotics were three hours late or omitted. Sterile field breached. Patient reported fever and increasing redness; nursing staff dismissed it as “normal healing” for 48 hours. By the time the surgeon was notified, the localized infection had become life threatening sepsis.
Blood Clot (DVT / Pulmonary Embolism)
Complication
Risk assessment performed. Compression devices applied. Blood thinners prescribed and administered on schedule. Clot formed despite full prophylaxis; a known outcome in approximately 3% of joint replacement patients.
Negligence
No risk assessment. No blood thinners despite documented obesity, cancer history, and prior clot. Nursing staff attributed severe calf pain to “normal post surgical pain.” Fatal pulmonary embolism.
Birth Injury (Shoulder Dystocia / Fetal Distress)
Complication
Shoulder dystocia occurred without warning. Obstetrician immediately executed the correct maneuvers in the correct sequence. Brachial plexus injury resulted despite a textbook response.
Negligence
Fetal monitor showed prolonged decelerations for over an hour. Staff ignored alarms. Provider applied excessive downward traction and contraindicated fundal pressure. Infant suffered hypoxic brain injury. Cerebral palsy.
Post Surgical Bleeding
Complication
Complex trauma surgery. Surgeon achieved hemostasis before closing. Patient developed coagulopathy from massive tissue damage. Team monitored drain output, tracked hemoglobin, and transfused appropriately.
Negligence
Routine gallbladder removal. Surgeon failed to properly clip the cystic artery. For four hours, nursing staff ignored plummeting blood pressure and spiking heart rate. Patient suffered brain damage from hypovolemic shock.
The Bottom Line for Patients
The injury itself does not determine whether you have a case. A blood clot can be bad luck or bad medicine. An infection can be unavoidable biology or a preventable protocol failure. What matters is whether the doctor followed the rules before, during, and after the event. That answer is in the medical record, and it takes an expert in the same specialty to extract it.
“NEVER EVENTS”: WHEN THERE IS NO DEBATE
Certain medical errors are universally classified by the medical community as indefensible. The National Quality Forum has identified 29 “Serious Reportable Events” that simply should not occur if basic safety protocols are followed. Under Florida Statute Section 395.0197, hospitals must report these to AHCA within 15 days. CMS will not reimburse hospitals for treating them.
These include: surgery performed on the wrong body part or wrong patient, a foreign object left inside the body after surgery, administration of the wrong drug or wrong blood type, infant discharged to the wrong person, Stage 3 or 4 pressure ulcers acquired after admission, and maternal death during a low risk pregnancy.
What This Means in Plain Terms
If the surgeon operated on the wrong body part, left an instrument inside you, gave you the wrong medication, or gave you someone else’s blood type; that is never a “complication.” The entire medical community agrees these should never happen. The federal government refuses to pay hospitals for treating the damage. If any of these happened to you, the debate is over before it starts.
If you suffered a catastrophic outcome and you are unsure whether it was a complication or negligence, contact the Law Offices of Jorge L. Flores, P.A. for a definitive answer.
Inside Advantage
Every defense starts with the same word: “complication.” Before founding this firm, Attorney Flores defended hospitals against exactly these claims from the other side of the table in Miami. He knows that the gap between “complication” and “negligence” is almost always found in the operational data the defense hopes no one subpoenas; the nursing flowsheet showing four hours of undocumented vital signs, the antibiotic administration log showing the prophylactic dose was three hours late, or the internal incident report the hospital’s own risk management team classified as a reportable adverse event. We build every case by extracting that data first.
Determining whether an injury meets the criteria of Section 766.102 requires a board certified medical expert in the exact same specialty. The Chapter 766 pre suit process mandates this review before a lawsuit can be filed. For the full analysis of recoverable damages and the economic viability threshold, see the linked guides.
If you suffered a catastrophic outcome and you are unsure whether it was a complication or negligence, the experienced Law Offices of Jorge L. Flores, P.A., can provide a definitive answer.
From our offices in Miami, Florida, we obtain the complete medical record, retain a board certified expert in the exact specialty, and apply the three question framework to give you a clear, honest evaluation. All costs are advanced by our firm, and no fee is charged unless we secure compensation.
P.S. The word “complication” appears in nearly every adverse event report a hospital generates. It is the default classification. But the timestamps, the nursing flowsheets, the medication logs, and the vital sign data already tell a different story. Call the Law Offices of Jorge L. Flores, P.A., today; because the answer to your question is already in the chart, and we know exactly where to find it.
Related: Medical Malpractice · Informed Consent · Surgical Errors · Hospital Negligence · Nursing Malpractice


