Reviewed by Jorge L. Flores, Esq. · Law Offices of Jorge L. Flores, P.A. · Miami, Florida · Last Updated: April 2026
Patients spend only a fraction of their hospitalization interacting with a physician. The vast majority of hands on, minute to minute clinical care; the medication dosages, the vital sign monitoring, the response to a deteriorating condition; is delivered by nurses. When a preventable nursing error results in permanent brain injury, paralysis, or death, the failure is not misfortune. It is accountability.
The Law Offices of Jorge L. Flores, P.A., in Miami, Florida, is a dedicated nursing malpractice law firm that understands both the clinical complexity and the profound human devastation that preventable nursing errors inflict upon patients and their families, and we are committed to providing aggressive, compassionate, and meticulous legal representation to victims of nursing negligence throughout the entire State of Florida.
Despite the prevalence of nursing negligence in hospitals, skilled nursing facilities, and long term care environments, it remains a heavily under examined category of medical malpractice. Patients and their families oftentimes operate under the generalized assumption that “the hospital made a mistake,” without understanding the specific, independent legal standards that govern nursing professionals or the intricate mechanisms through which a hospital or corporate nursing home is held financially accountable for a nurse’s error under Florida law.
~10,000
Estimated Annual Deaths From Medical Errors in Florida
70%+
Of Bedside Care Delivered by Nursing Staff, Not Physicians
2 Years
Florida Statute of Limitations for Nursing Malpractice Claims
Sources: Institute of Medicine, National Academy of Sciences · Florida Statute Section 95.11
IS YOUR LOVED ONE STILL IN THE HOSPITAL OR NURSING FACILITY
If you are reading this page because a nurse’s error has just harmed someone you love and they are still receiving care, there are steps you should take right now to protect their rights and preserve the evidence.
Do not sign anything presented by the hospital’s risk management team without consulting an attorney first. Request a complete copy of the medical record in writing today; not through the patient portal, which omits critical nursing flowsheets and audit trail data.
Photograph any visible injuries including bruises, surgical sites, IV infiltration burns, or pressure wounds with your phone and include the date. Write down the name of every nurse and physician you can remember who was involved in your loved one’s care.
Do not discuss the details of what happened with hospital administrators, patient advocates, or risk management representatives; their role is to protect the hospital, not your family. If the situation involves a nursing home, contact the Florida Agency for Health Care Administration complaint line at (888) 419-3456 to file a formal report. Then call an attorney who will issue a records preservation letter before routine IT processes overwrite the electronic evidence.
WHAT IS NURSING MALPRACTICE UNDER FLORIDA LAW
Nursing malpractice occurs when a licensed nursing professional deviates from the prevailing professional standard of care recognized within the nursing community, and that deviation proximately causes injury, harm, or death to a patient who was under the nurse’s direct or indirect clinical supervision. Under Section 766.102 of the Florida Statutes, the prevailing professional standard of care is strictly defined as the level of care, skill, and treatment that a reasonably prudent nurse with similar training, education, and experience would provide under the same or similar clinical circumstances.
It is significant to note that nursing malpractice is legally and clinically distinct from physician malpractice, because nurses are governed by an entirely separate statutory framework under Chapter 464 of the Florida Statutes; the Florida Nurse Practice Act; and are held to professional standards specific to their licensure level, their clinical specialty, and the particular healthcare environment in which they practice. A registered nurse working in a cardiovascular intensive care unit is judged solely by what a reasonably prudent cardiovascular intensive care nurse would do under identical clinical circumstances; not by the standard of a physician, a surgeon, or a hospital administrator.
Florida Statute Section 766.102
The injured party bears the burden of proving by the “greater weight of the evidence” that the nurse’s actions represented a breach of the prevailing professional standard of care and that the breach was the proximate cause of the resulting injury. The mere existence of a poor clinical outcome does not automatically create an inference or presumption of negligence.
NURSING JUDGMENT VS. MEDICAL JUDGMENT
Defense attorneys in nursing malpractice litigation frequently attempt to deflect liability away from the nurse and onto the attending physician, arguing that the nurse was merely “following orders” and therefore cannot be held independently responsible for the patient’s harm. This narrative fundamentally misrepresents the legal obligations imposed upon nursing professionals under the Florida Nurse Practice Act.
The nursing standard of care demands independent clinical judgment, critical assessment, and active patient advocacy that extends well beyond the passive execution of physician directives. If a physician issues an order that a reasonably prudent nurse would recognize as dangerously erroneous, the nurse has an affirmative legal duty to question that order and, if necessary, refuse to carry it out.
|
PHYSICIAN MALPRACTICE A doctor misdiagnoses a patient’s condition and prescribes the wrong medication for that condition. The resulting harm constitutes physician malpractice because the error lies in the medical diagnosis. |
NURSING MALPRACTICE A doctor prescribes the correct medication, but the nurse administers it via the wrong route; intravenously instead of orally. The resulting harm constitutes nursing malpractice because the error lies in the nurse’s execution of their independent clinical duty. |
Furthermore, and this is a distinction that oftentimes proves decisive in complex nursing negligence litigation, the nurse’s duty of assessment is entirely independent of the physician’s diagnostic role. If a nurse observes that a patient is exhibiting acute cyanosis, a rapidly dropping blood pressure, and an escalating respiratory rate but fails to notify the physician or activate the clinical chain of command, that failure constitutes nursing malpractice; irrespective of whether the physician’s underlying diagnosis was correct.
If a nursing error has caused catastrophic harm to you or a loved one, contact the Law Offices of Jorge L. Flores, P.A. for a free consultation.
THE MOST COMMON TYPES OF NURSING MALPRACTICE
The clinical responsibilities assigned to nursing professionals make them the final safeguard between a patient and a catastrophic outcome, and when that safeguard fails, the resulting injuries are oftentimes severe, permanent, and life-altering.
|
Medication Errors Violations of the universal Five Rights; wrong patient, wrong drug, wrong dose, wrong route, wrong time. Includes decimal point errors that are particularly fatal in pediatric care, failure to check documented allergies, and improperly programmed IV infusion pumps delivering uncontrolled bolus doses of Heparin, Insulin, or Potassium Chloride. |
Failure to Monitor and Assess Recording vital signs without recognizing that incrementally worsening data represents the onset of sepsis, internal hemorrhaging, or respiratory failure. Includes ignoring or silencing telemetry alarms; a phenomenon known as “alarm fatigue”; and failure to perform ordered neurological assessments on head trauma patients. |
Failure to Escalate If a physician is unresponsive, dismissive, or provides an order the nurse recognizes as inadequate, the nurse has a legal duty to escalate the issue up the clinical chain of command; to the charge nurse, nursing supervisor, rapid response team, and chief medical officer. Silence in the face of patient decline is a breach of duty. |
|
Patient Falls Catastrophic hip fractures, femur fractures, and subdural hematomas resulting from the failure to administer a validated fall risk assessment, activate bed alarms, or provide direct physical assistance during ambulation; particularly devastating in Florida’s vast geriatric population. |
Pressure Ulcers (Bedsores) Advanced Stage 3 and Stage 4 pressure ulcers are classified as “never events” by Medicare. The presence of deep wounds involving exposed bone, tendon, or muscle in a facility is considered glaring, undeniable proof of prolonged nursing neglect and a severe breach of the standard of care. |
IV and Catheter Injuries IV extravasation of vesicant medications causing severe chemical burns, tissue necrosis, or amputation. Catheter-associated urinary tract infections (CAUTI) and central line-associated bloodstream infections (CLABSI) from failure to utilize sterile technique. Restraint injuries from improper application or failure to perform neurovascular checks. |
What This Means for Patients
If your condition worsened because a nurse gave the wrong medication, missed deteriorating vital signs, failed to call the doctor when something was clearly wrong, or did not reposition you frequently enough to prevent bedsores, those are not unfortunate accidents. They are failures to perform fundamental nursing duties that the law requires. The hospital that employed the nurse is financially responsible.
Red Flags That Suggest Nursing Negligence, Not Bad Luck
Most families cannot diagnose malpractice from the bedside. However, certain behavioral and situational patterns consistently appear in cases that turn out to involve nursing negligence rather than an unavoidable medical outcome. If you observed any of the following, the medical record deserves an independent expert review.
☐ The nurse who was caring for your loved one was suddenly reassigned to a different unit after the incident, or you never saw them again without explanation.
☐ A hospital administrator, patient advocate, or risk management representative visited your family unsolicited to “explain what happened” or offer condolences before you asked any questions.
☐ You noticed long gaps between call light activation and a nurse responding; or your loved one reported pressing the call button repeatedly with no response during the hours before the event.
☐ The hospital offered to waive certain bills, reduce your charges, or provide free follow up care without being asked.
☐ You were told the event was a “known complication” but the consent form your loved one signed does not list that specific outcome.
☐ The physician who had been managing your loved one’s care was suddenly replaced by a new doctor you had never met.
☐ You noticed that the condition of your loved one changed dramatically during a night shift, weekend, or holiday; when staffing levels are at their lowest.
☐ The nursing notes in the patient portal appear unusually brief, vague, or generic for the hours surrounding the event.
None of these indicators prove malpractice on their own. But each one is a pattern that the Law Offices of Jorge L. Flores, P.A., has seen repeatedly in cases where the EHR audit trail ultimately revealed a nursing failure that the facility attempted to minimize.
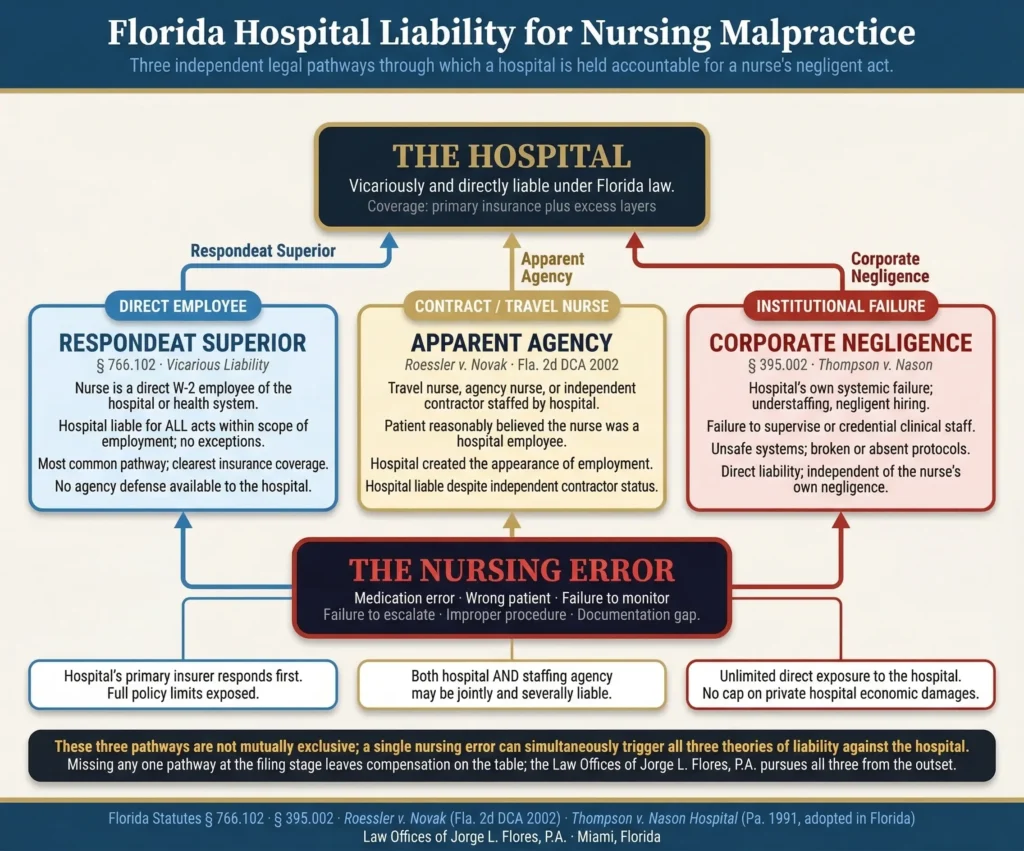
WHY BOTH THE NURSE AND THE HOSPITAL ARE ACCOUNTABLE
When nursing negligence results in catastrophic injury or death, the most critical question for the injured family becomes one of financial recovery. Individual nurses rarely carry sufficient personal malpractice insurance to compensate a plaintiff for permanent brain injury, loss of future earning capacity, and a lifetime of rehabilitative care. Therefore, nursing malpractice litigation in Florida relies heavily on proving that the medical facility; which possesses deep corporate insurance policies and substantial institutional assets; is legally responsible for the nurse’s failure.
|
Respondeat Superior When the negligent nurse is a direct W-2 employee of the hospital and commits malpractice while executing their assigned job duties, the hospital is strictly liable for the resulting harm. The plaintiff is not required to prove the hospital itself acted negligently; the employee’s error imputes full liability to the facility. |
Apparent Agency Florida’s post-COVID healthcare system relies heavily on traveling nurses and contract staffing agencies. When a travel nurse wearing hospital scrubs and using hospital equipment commits malpractice, Florida courts oftentimes hold the hospital vicariously liable under the doctrine of apparent agency; because the patient had no realistic way to verify the nurse’s employment status. |
Corporate Negligence Holds the hospital directly liable for its own systemic failures, including, but not limited to, intentional understaffing below safe ratios, negligent hiring or retention of nurses with documented disciplinary histories, failure to implement evidence-based clinical protocols, and failure to supervise newly graduated or float pool nurses. |
NURSING HOME MALPRACTICE AND CHAPTER 400
Given Florida’s massive elderly demographic and its status as the state with the highest concentration of geriatric population in the country, a significant proportion of nursing negligence occurs within skilled nursing facilities, assisted living facilities, and long term care environments. These claims are oftentimes pursued under the authority of Florida Statute Chapter 400, which codifies the Nursing Home Residents’ Bill of Rights; a statutory pathway that allows families to hold the corporate facility accountable for failures resulting in dehydration, malnutrition, unassisted falls, and pressure ulcers without necessarily navigating the complex procedural hurdles of Chapter 766 medical malpractice litigation.
Florida’s Mandatory Nursing Home Staffing Ratios — Section 400.23
Florida law mandates that nursing homes provide a minimum of 3.6 hours of direct care per resident per day, including at least 2.0 hours from a Certified Nursing Assistant and 1.0 hour from a licensed nurse. Facilities cannot operate with a ratio worse than one CNA per 20 residents or one licensed nurse per 40 residents at any time. When investigating a nursing home injury, the Law Offices of Jorge L. Flores, P.A., immediately subpoenas the facility’s master staffing logs, payroll records, and federal CMS data to determine whether the facility was operating below these statutory minimums at the time the resident was harmed.
The root cause of almost all nursing home negligence in Florida is severe, calculated understaffing by corporate owners who minimize staffing levels to maximize profit margins, leaving skeleton crews of underpaid nurses and CNAs to care for dozens of highly acute, dependent residents. If the staffing data proves the facility was violating Section 400.23, the narrative presented to a jury shifts from a single overworked CNA making a mistake to a corporate entity knowingly violating state law and prioritizing profit margins over legally mandated resident safety.
The Bottom Line on Nursing Home Cases
If a nursing home resident suffered a preventable fall, developed severe bedsores, or was found dehydrated or malnourished, the first question is not whether one nurse made a mistake. The first question is whether the facility had enough staff on the floor to provide legally mandated care. The staffing logs answer that question, and we subpoena them immediately.
EHR AUDIT TRAILS: THE SILENT WITNESS
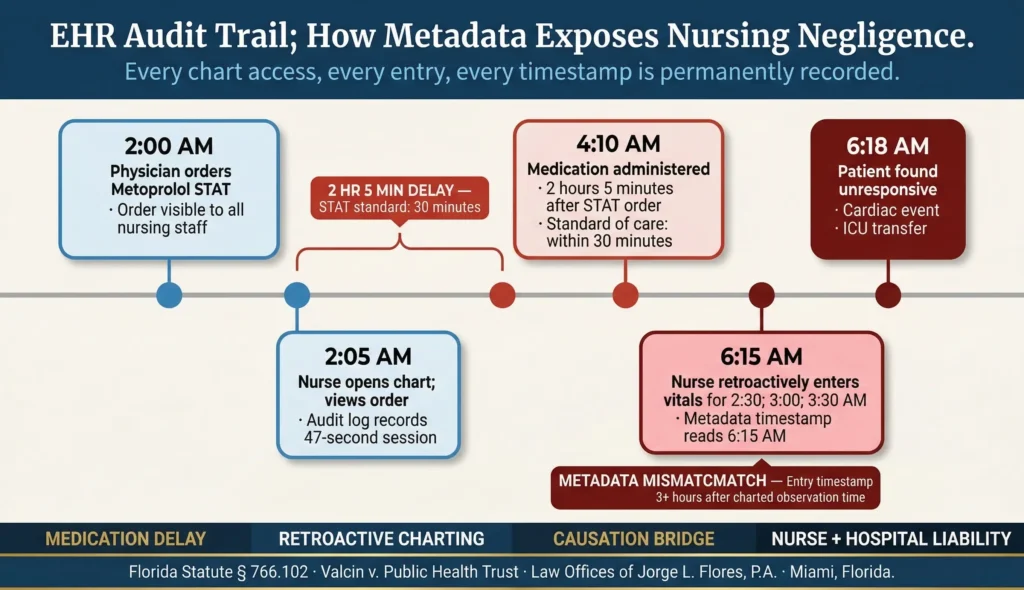
The foundational maxim in nursing education is this; if it was not documented, it was not done. In contemporary nursing malpractice litigation, the most devastating and undeniable evidence of negligence is oftentimes found not in the visible patient chart but hidden within the metadata of the Electronic Health Record; known as the audit trail.
Under Section 766.204 of the Florida Statutes, healthcare facilities are legally required to produce all relevant medical records within ten business days of a formal request. Experienced malpractice attorneys at the Law Offices of Jorge L. Flores, P.A., petition courts to mandate the inclusion of the complete EHR audit trail; a sequential, time-stamped background log that records every single digital interaction with a patient’s electronic file, including exactly which user opened the chart, the precise second they accessed it, and exactly what data they entered, modified, or deleted.
| Timestamp | User ID | Action | What the Audit Trail Reveals |
|---|---|---|---|
| 02:00 AM | MD_Jones | Order Entry | Physician orders urgent IV Heparin bolus |
| 02:05 AM | RN_Smith | View Order | Nurse views the urgent medication order |
| 04:10 AM | RN_Smith | Execute Medication | Nurse charts Heparin as administered; metadata proves a lethal 2 hour delay in execution |
| 06:15 AM | RN_Smith | Late Entry | Nurse retroactively charts vitals for 03:00, 04:00, and 05:00 at 6:15 AM |
| 06:18 AM | RN_Smith | Code Blue Note | Patient found unresponsive; metadata exposes fraudulent retroactive charting to conceal failure to monitor |
This audit trail serves as an unblinking, objective silent witness that regularly destroys defense narratives. If a nurse testifies under oath that they were physically at the bedside performing hourly neurological assessments, but the audit trail metadata proves the nurse’s unique login was actively charting on entirely different patients in a different wing of the hospital during that exact timeframe, the nurse’s credibility is irrevocably shattered and the case pivots decisively in favor of the injured patient and family.
This Evidence Has an Expiration Date
Hospital EHR systems run automated data retention protocols that routinely purge audit trail metadata after defined periods. Once overwritten, the digital forensic evidence that proves when a chart entry was actually made; as opposed to when it claims to have been made; is gone permanently. A records preservation letter sent by an attorney creates a legal duty for the hospital to halt all deletion and secure every record, audit trail, and piece of equipment related to your loved one’s care. If evidence disappears after the hospital receives that letter, the court can instruct the jury to presume the destroyed data proved negligence. This is why the first 48 to 72 hours after a nursing injury matter more than any other window in the case.
Inside Advantage
Attorney Flores also worked as an attorney for a top rated insurance defense firm in Miami, where he learned first hand how hospitals and their insurers defend nursing malpractice claims. He understands precisely how defense counsel deploys the “unavoidable complication” argument; attributing catastrophic outcomes to the patient’s underlying comorbidities rather than to documented nursing failures. He knows how defense experts are retained, how nursing records are reframed, and how risk management teams attempt to minimize institutional exposure during the mandatory pre suit period. This inside knowledge gives the Law Offices of Jorge L. Flores, P.A., a significant tactical advantage; because we do not simply build a case for our client. We build it with a complete understanding of how the other side intends to dismantle it.
FLORIDA’S COMPENSATION LANDSCAPE
Under Florida law, victims of nursing malpractice may be entitled to recover damages, including, but not limited to, compensation for past and future medical expenses, hospitalization and rehabilitation costs; lost income, future earnings, and disability benefits; and the profound physical pain, mental anguish, and loss of the capacity for the enjoyment of life suffered by the patient and their family.
It is significant to note that the corporate status of the defendant hospital is one of the most financially consequential factors in every nursing malpractice case we evaluate. For claims against private hospitals, the Florida Supreme Court struck down non-economic damage caps as unconstitutional; meaning there is no statutory ceiling on what a jury may award for pain and suffering. However, if the negligence occurred at a government-owned public hospital, damages are strictly capped under sovereign immunity at $500,000 per person for claims accruing between October 2026 and September 2031. This distinction can represent millions of dollars in recoverable compensation, and it is one of the first determinations we make in every case.
Florida’s “Free Kill” Law — Section 768.21(8)
If an unmarried adult patient over the age of 25 with no minor children dies due to nursing negligence, the patient’s surviving parents and adult children are legally barred from recovering non-economic pain and suffering damages. Florida remains the only state in the nation with this specific restriction. Despite overwhelming bipartisan support for repeal in 2025 and 2026, the legislation was vetoed and this devastating barrier remains active law. The Law Offices of Jorge L. Flores, P.A., navigates this complex statutory landscape on behalf of every client and works diligently to identify all available avenues of recovery.
PRE-SUIT REQUIREMENTS AND STATUTE OF LIMITATIONS
Florida law imposes some of the most rigorous procedural requirements in the nation upon plaintiffs who seek to file nursing malpractice claims, and the failure to strictly adhere to each step will result in the immediate dismissal of the case regardless of the severity of the nursing negligence.
Step 01 — Expert Affidavit
Secure a verified written affidavit from a qualified medical expert; a nurse practicing in the same clinical specialty as the defendant; confirming that the standard of care was breached and caused the injury. A physician, hospital administrator, or surgeon cannot generally serve as the sole expert establishing a breach of the nursing standard.
Step 02 — Notice of Intent
Serve a formal Notice of Intent to Initiate Litigation upon the nurse and the hospital, triggering a mandatory 90 day pre suit screening period during which the statute of limitations is tolled and the hospital’s risk management team conducts its own investigation.
Critical Deadline — Florida Dual Clock System
Florida enforces a strict two year statute of limitations from the date the injury was discovered or reasonably should have been discovered, and a strict four year statute of repose from the date the negligent act occurred; regardless of when the injury was finally identified. Because the mandatory pre suit process requires a minimum of 90 days plus the time to secure an expert affidavit, consulting with a specialized nursing malpractice attorney at the Law Offices of Jorge L. Flores, P.A., as soon as possible is a time-sensitive imperative. Do not delay. The clock is running.
WE ARE PREPARED TO PURSUE YOUR CLAIM
If you or a loved one has been seriously injured or has suffered the death of a family member as a result of nursing malpractice in a Florida hospital, nursing home, or long term care facility, the experienced Law Offices of Jorge L. Flores, P.A., can help.
From our offices in Miami, Florida, we retain the best same-specialty nursing experts, medical investigators, and legal professionals in the field to forensically deconstruct clinical timelines, secure and decode raw electronic health record audit trails, and build the strongest possible case on your behalf. We prepare for every case with the understanding that it will be tried before a jury, and we will work tenaciously to obtain the maximum compensation available under the law for you and your family.
P.S. Florida nursing malpractice cases are won or lost in the immediate aftermath of the injury. Large hospitals and corporate nursing homes maintain sophisticated risk-management teams designed to minimize institutional liability the exact moment an adverse event occurs. At the Law Offices of Jorge L. Flores, P.A., we move immediately to secure complete medical records, demand the native EHR audit trails, subpoena staffing logs and pharmacy dispensing data, and retain same-specialty nursing experts; because a case built on mathematical certainty from electronic metadata is a case that defense counsel cannot dismantle. Call today; because we believe you deserve an honest answer about whether you have a viable claim.
Related: Medical Malpractice · Who Can Be Held Responsible · Complication vs. Negligence · Medical Records Guide · Wrongful Death


