Reviewed by Jorge L. Flores, Esq. · Law Offices of Jorge L. Flores, P.A. · Miami, Florida · Last Updated: March 2026
You went in for a surgery that was supposed to help you. You came out with an injury that was not there before. And when you asked what happened, the surgeon told you it was a “known complication.” It was not.
The profound vulnerability of undergoing surgery; being rendered unconscious, chemically paralyzed, and entirely dependent on the expertise, vigilance, and communication of a medical team; makes a surgical error one of the most traumatic forms of medical malpractice we encounter at the Law Offices of Jorge L. Flores, P.A.
When that trust is breached, a patient may wake up with a visible deformity, complete loss of motor function, chronic debilitating pain, or the sudden realization that they require immediate corrective surgery to save their life. From our offices in Miami, Florida, we have represented surgical error victims throughout the entire State of Florida, and we understand both the clinical complexity of these cases and the deeply personal toll they exact on patients and their families.
DID YOU JUST WAKE UP FROM SURGERY WITH AN UNEXPECTED INJURY
If you are reading this page because you or a loved one has just experienced an unexpected surgical outcome and you suspect something went wrong in the operating room, take these steps now.
Do not accept the explanation that it was a “known complication” without an independent review of the operative report by a qualified expert.
Request your complete medical record in writing today; specifically the operative report, the anesthesia record, and the nursing intraoperative notes. Do not rely on the patient portal; it omits critical surgical documentation.
Do not sign any documents presented by the hospital’s risk management team, patient relations department, or billing office without consulting an attorney.
Photograph any visible injuries including incision sites, bruising, swelling, drainage, or deformity. Write down everything you remember the surgical team telling you before and after the procedure. If you are still in the hospital, ask the charge nurse for the name of every surgeon, anesthesiologist, and surgical assistant who was present in the operating room.
MEDICAL GASLIGHTING VS. ACTUAL NEGLIGENCE
When a surgical complication arises, the immediate, almost reflexive response from the surgical team is to point to the informed consent documentation. You are routinely told, “We discussed this risk before surgery; you signed the form acknowledging that this was a known complication.” However, a critical distinction exists in both medicine and law between an inherent surgical risk and a negligently caused injury; and understanding this distinction is the foundational step in determining whether you have a viable medical malpractice claim under Florida law.
Inherent Surgical Risk
A complication that can occur even when the surgeon executes every step flawlessly, adhering strictly to the prevailing standard of care. Examples include a certain degree of unavoidable bleeding, a low grade post operative infection, or the formation of internal scar tissue despite immaculate surgical technique and sterile protocols.
Negligently Caused Injury
An injury that directly results from a deviation from the standard of care. If a surgeon severs a major nerve because they failed to properly identify anatomical landmarks, or punctures an organ because they inserted an instrument with excessive, uncontrolled force; that is not an inherent risk. That is actionable surgical negligence.
A patient consents to the unavoidable risks of a properly and competently performed surgery; they do not, and cannot, consent to substandard care, reckless surgical technique, or blatant medical negligence. If a bowel is perforated during laparoscopy because a trocar was inserted without proper pneumoperitoneum or without utilizing the camera for direct visualization, the injury transitions from a “known risk” to irrefutable malpractice. For a deeper analysis of the legal distinction between complications and negligence, including the consent form myth, see our complication vs. negligence guide.
It is significant to note that the failure to recognize and repair a complication during the initial surgery is oftentimes considered a separate, distinct act of negligence. A bowel perforation that is immediately identified and carefully sutured during the operation may represent standard clinical management. However, discharging a patient with an unrecognized, leaking perforation; ignoring their escalating complaints of severe abdominal pain, tachycardia, and fever; and allowing the patient to slowly develop life threatening septic shock represents a catastrophic, multi level failure of care that constitutes egregious medical malpractice.
WHY SURGICAL MISTAKES HAPPEN
75%
Of Surgical Malpractice Cases Involve Intraoperative Error
50%
Of Waking Hours Surgeons Report Significant Fatigue
$3.8B
Annual U.S. Payouts for Surgical Malpractice Claims
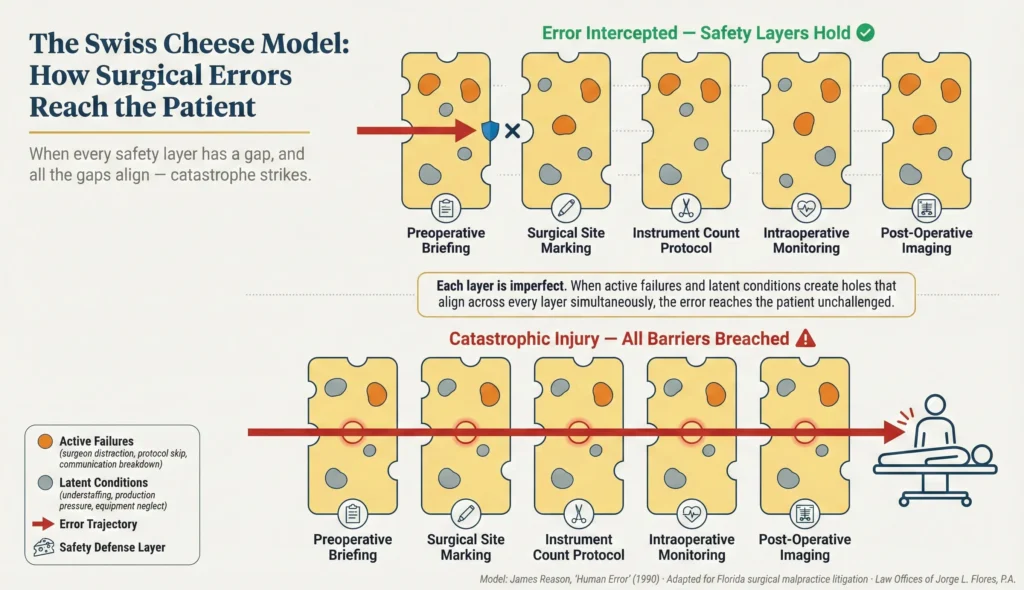
Intraoperative errors are estimated to be the primary, driving issue in 75% of all medical malpractice cases involving surgeons. These are not random acts of fate. They are the predictable, preventable results of systemic breakdowns, human error, and cultural failures within the high stakes environment of the operating room. Patient safety experts utilize the “Swiss Cheese Model,” developed by cognitive psychologist James Reason, to explain how catastrophic surgical mistakes reach the patient despite multiple layers of defense.
In a modern hospital system, there are multiple, redundant layers of defense designed specifically to protect the patient from harm; preoperative briefings, standardized site markings, electronic medical records, rigid instrument counting protocols, and post operative imaging. However, each layer of defense is imperfect. Much like a slice of Swiss cheese, every safety protocol has “holes” representing distinct vulnerabilities. When the holes align across multiple layers simultaneously, the error breaches every single safety barrier and strikes the patient.
The ingrained culture of the operating room heavily influences the frequency and severity of surgical errors. The traditional, rigid hierarchy of the operating theater can be clinically lethal. When an environment is dominated by an authoritarian, unapproachable lead surgeon, the subordinate staff; including highly trained nurses, surgical technicians, and junior residents; oftentimes experience what clinical researchers describe as severe “hierarchy problems.” They become paralyzed by professional fear, hesitant to speak up when they witness a clear deviation from standard protocols. This culture of silence actively disables the redundant safety checks designed to protect you.
Surgeon fatigue is another pervasive, highly dangerous factor that we scrutinize in virtually every surgical malpractice investigation we conduct at the Law Offices of Jorge L. Flores, P.A. Extensive clinical studies reveal that surgeons can be significantly fatigued for up to 50% of their waking hours. Research demonstrates that sustained wakefulness of 24 hours results in a measurable decline in cognitive processing and psychomotor performance that is functionally equivalent to a blood alcohol concentration of 0.10%; a level of impairment well above the legal limit for operating a motor vehicle. Yet these same impaired individuals are legally permitted to operate on human beings. As a surgeon moves to their third or fourth complex case of the day, “decision fatigue” severely depletes their mental resources, increasing reliance on dangerous heuristics and faster, riskier maneuvers simply to finish the procedure.
What This Means for Patients
Surgical errors are not caused by a single person making a single mistake. They happen when multiple safety systems fail at the same time; a tired surgeon, a nurse afraid to speak up, a skipped checklist step, and a hospital that scheduled too many procedures in one day. Understanding this is important because the defense will try to blame one individual. We investigate the entire chain.
NEVER EVENTS: THE UNFORGIVABLE FAILURES
Within the clinical, regulatory, and legal communities, there is a specific classification of surgical errors so egregious, so unequivocally preventable, and so devastating that the National Quality Forum officially designates them as “Never Events.” The Centers for Medicare and Medicaid Services takes these events so seriously that it refuses to reimburse hospitals for the costs associated with treating the aftermath of these specific errors; forcing the hospital to absorb the financial burden of its own negligence.
Wrong Site Surgery
Performing an incision, amputation, or invasive procedure on the incorrect side of the body or the entirely wrong anatomical location.
Wrong Patient Surgery
Performing a procedure intended for one patient on a completely different, unsuspecting individual due to a catastrophic failure in basic identification protocols.
Wrong Procedure
Performing an entirely unintended surgery on a patient; for example, performing a hysterectomy when the patient was scheduled for a simple appendectomy.
Retained Foreign Objects
Leaving surgical sponges, heavy cotton towels, sharp needles, or metallic instruments inside a patient’s body cavity after the wound is closed.
Under Section 766.102(3)(b) of the Florida Statutes, the discovery of a retained foreign object inside a patient’s body establishes a mandatory presumption of negligence. The Florida Supreme Court affirmed in Dockswell v. Bethesda Memorial Hospital that this presumption is absolute, requiring the jury to receive a specific instruction establishing negligence regardless of whether there is direct evidence of who on the surgical team left the object behind. For other Never Events, the doctrine of res ipsa loquitur (“the thing speaks for itself”) provides a powerful evidentiary inference of negligence when the patient was unconscious and the instrumentality was under the exclusive control of the surgical team.
If you suspect that a surgical error caused your injury, contact the Law Offices of Jorge L. Flores, P.A. for a confidential consultation before critical evidence is lost.
THE 19 STEP SAFETY CHECKLIST THEY WERE REQUIRED TO FOLLOW
To combat the prevalence of surgical errors and Never Events, the global medical community established mandatory, standardized pre surgical safety protocols. Foremost among these are the Joint Commission’s Universal Protocol and the World Health Organization Surgical Safety Checklist. When an operating room team fails to meticulously complete every single step of these protocols, it provides near automatic, compelling evidence of medical negligence. Before your surgery, these 19 steps were strictly required to occur.
Phase 1: Sign In (Before Anesthesia)
1. Has the patient confirmed identity, site, procedure, and consent? You must be awake and asked to explicitly state your name and what surgery you are having.
2. Is the site marked? The surgeon must physically draw on your skin where the cut will be made.
3. Is the anesthesia machine and medication check complete?
4. Is the pulse oximeter on the patient and functioning?
5. Does the patient have a known allergy? The team must verbally verify all critical drug allergies.
6. Difficult airway or aspiration risk? Backup emergency equipment must be prepared.
7. Risk of greater than 500ml blood loss? Rapid IV fluids and blood products must be immediately available.
Phase 2: Time Out (Before Skin Incision)
8. Confirm all team members have introduced themselves by name and role. This breaks dangerous, silent hierarchies.
9. Confirm patient’s name, procedure, and where the incision will be made. The final collective verbal pause before the scalpel touches tissue. If an error occurs after this step, the Time Out was skipped or rushed.
10. Has antibiotic prophylaxis been given within the last 60 minutes? Vital evidence in post operative sepsis and MRSA cases.
11. Surgeon anticipated critical events: critical steps, duration, expected blood loss.
12. Anaesthetist anticipated critical events: patient specific heart, lung, or metabolic concerns.
13. Has sterility been confirmed, including indicator results?
14. Are there equipment issues or any concerns?
15. Is essential imaging displayed? Operating without imaging leads directly to anatomical disorientation and wrong site surgery.
Phase 3: Sign Out (Before Leaving the Operating Room)
16. Nurse verbally confirms the name of the procedure.
17. Completion of instrument, sponge, and needle counts. The final count must perfectly match the starting count before the patient is closed; the primary defense against retained foreign objects.
18. Specimen labelling; read aloud, including patient name. Prevents mislabeled cancer biopsies and unnecessary chemotherapy.
19. Key concerns for recovery and management of this patient. Essential for proving negligence when patients hemorrhage or stop breathing in the recovery room.
HOW TO READ YOUR OPERATIVE REPORT
If you suspect you are the victim of a surgical error, the single most critical document in your entire medical chart is the operative report. This document is the official, dictated account of what transpired in the operating room from the first incision to the final suture. You have an absolute, undeniable right to obtain it under HIPAA and Florida law. However, because surgeons are acutely aware that this document is a binding legal record, it is oftentimes heavily sanitized, strategically worded, or deliberately vague. At the Law Offices of Jorge L. Flores, P.A., we know exactly how to dissect an operative report to uncover the hidden markers of negligence.
Red Flags in the Operative Report
☐ “Complications Encountered” buried deep within the “Findings” or “Description of Procedure” sections rather than stated clearly in the heading.
☐ “Unusual Anatomy” or “Dense Adhesions” used to blame alleged anatomical abnormalities for poor visualization. If visibility was severely compromised, the standard of care requires the surgeon to halt, alter their approach, or call for a specialized consult. ☐ Disproportionate Operative Times. If a routine 45 to 90 minute procedure spanned 3 to 4 hours, it is a glaring indicator that a catastrophic error occurred and the team spent hours attempting to control unexpected hemorrhage or repair damaged structures.
☐ Conversion from Minimally Invasive to Open Surgery. If your laparoscopy was suddenly converted to an open laparotomy requiring a massive abdominal incision, a major vascular injury or organ perforation likely occurred.
☐ High Estimated Blood Loss documented in the report indicates an unintended arterial or venous laceration during the dissection.
☐ Vague Language or Unexplained Deviations. Descriptions that lack anatomical specificity or gloss over critical steps of the surgical dissection are highly suspicious. What the surgeon fails to write is oftentimes just as important as what they include.
How to Use This Information
Request the complete operative report from the hospital in writing. Read it carefully and look for the red flags above. If you see any of them; particularly a procedure that took far longer than expected, a conversion to open surgery, or vague language where anatomical specificity should be; bring the report to an attorney who handles surgical malpractice. The operative report is the surgeon’s own account of what happened, and it is the first document our experts review.
HIGH RISK SURGERIES AND SPECIFIC COMPLICATIONS
While surgical errors can happen during any procedure, certain complex surgeries carry inherently elevated risks for devastating, specific types of malpractice. At the Law Offices of Jorge L. Flores, P.A., we have extensive experience investigating and litigating cases involving the following high risk surgical categories.
Spinal Surgery: Nerve Damage and Paralysis
Laminectomies, spinal fusions, and microdiscectomies demand extraordinary anatomical precision. Even a millimeter of deviation can result in permanent paralysis, chronic intractable radiculopathy, or complete loss of bowel and bladder control. Common litigated errors include improper placement of pedicle screws, failure to identify and repair a dural tear before closing, and operating on the wrong spinal level.
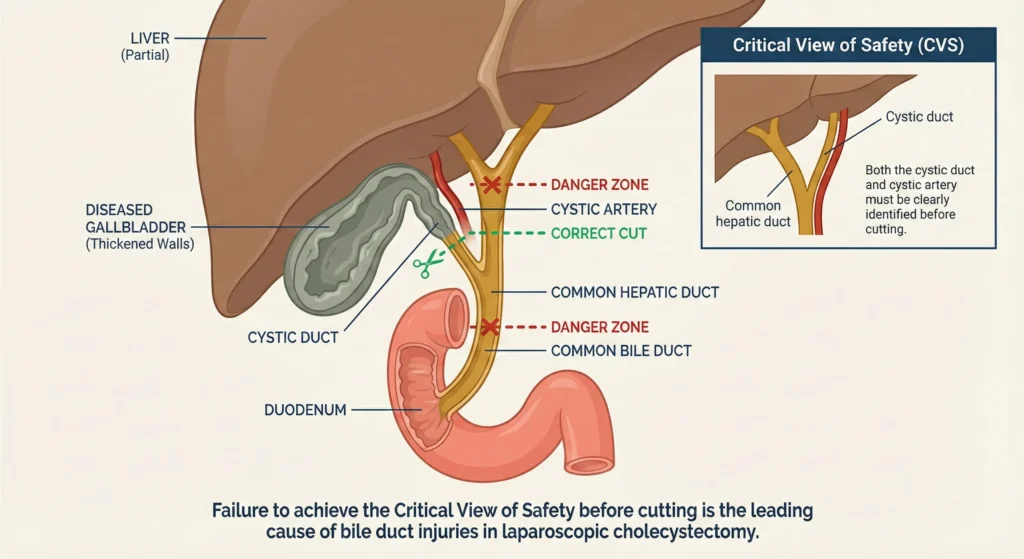
Laparoscopic Cholecystectomy: Bile Duct Injuries
The removal of the gallbladder is one of the most common surgeries performed worldwide, but it carries the risk of catastrophic bile duct injury when the surgeon fails to establish the “Critical View of Safety”; a mandatory visual verification standard. A mistakenly severed common bile duct leaks highly caustic bile directly into the sterile abdominal cavity, causing severe biliary peritonitis and requiring highly complex reconstructive surgery that carries a 10% to 20% risk of long term strictures and lifelong liver infections.
Hysterectomy and Gynecological Surgery: Ureteral Injuries
During major pelvic surgeries, the ureters are in extreme danger. Clinical data reveals that up to 70% of ureteral injuries are completely missed during the operation. Patients are discharged, only to return to the emergency room days later presenting with severe flank pain, uncontrollable fever, and toxic urinary leakage. Approximately 77% require major reconstructive reoperation, and up to 10% suffer the permanent, irreversible loss of a kidney.
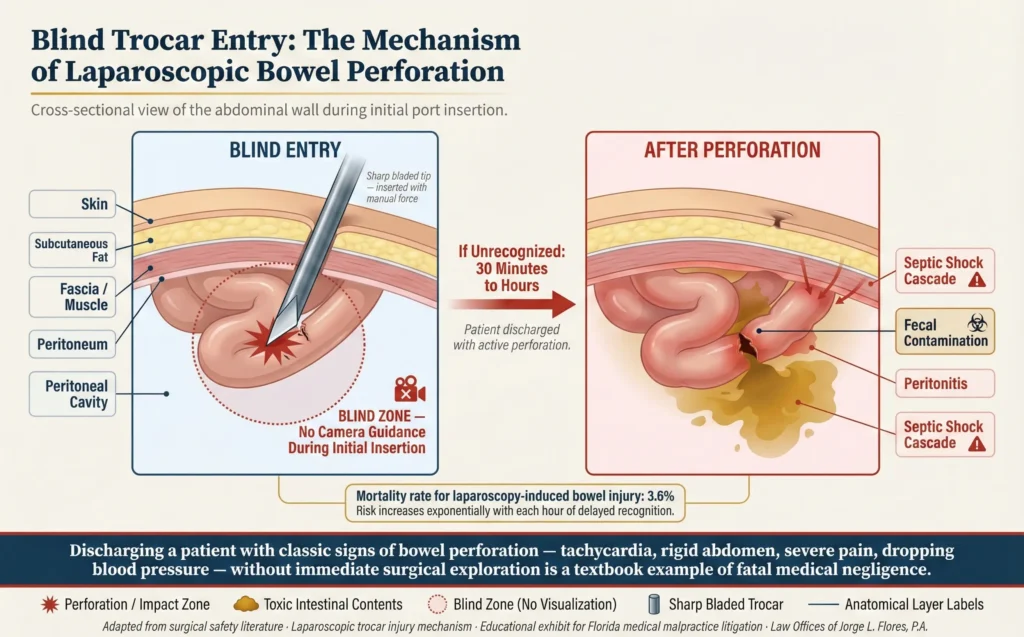
General Laparoscopy: Bowel Perforations
Laparoscopic surgery involves inserting sharp, bladed trocars forcefully into the abdomen, and the initial insertion is frequently performed “blindly” without direct camera visualization, placing the bowel at constant risk. A perforated bowel leaks highly toxic contents directly into the sterile abdominal cavity, triggering rapid, life threatening peritonitis and septic shock. Discharging a patient who exhibits the classic signs of a perforation; tachycardia, a rigid abdomen, agonizing pain, and dropping blood pressure; without immediate surgical exploration is a textbook example of fatal medical negligence. The mortality rate associated with laparoscopy induced bowel injury remains unacceptably high at 3.6%.
The Operative Report Has an Expiration Date
Surgeons typically dictate the operative report within 24 hours of the procedure. However, the EHR audit trail oftentimes reveals that the report was modified, amended, or entirely re-dictated days or weeks later; after the hospital’s risk management team identified the legal exposure. A records preservation letter sent by an attorney within the first 48 to 72 hours creates a legal duty for the hospital to preserve the original dictation, all subsequent modifications, and the complete audit trail. If the hospital destroys or overwrites this evidence after receiving the letter, the court can instruct the jury to presume the original report proved negligence.
Inside Advantage
Attorney Flores worked as an attorney for a top rated insurance defense firm in Miami, where he learned first hand how defense attorneys construct the narrative around surgical errors. He knows how the operative report is used to reframe a preventable mistake as an “inherent risk.” He knows how defense experts are selected specifically to testify that the complication was unavoidable. And he knows how the complication defense is built from the first phone call the hospital’s risk manager makes to outside counsel. That experience is why every surgical malpractice case we build is constructed not just to prove what the surgeon did wrong, but to preemptively disarm the defense narrative the hospital began constructing the moment the patient was wheeled out of the operating room.
Florida law requires a mandatory pre suit investigation before a surgical malpractice lawsuit can be filed. The corroborating expert must be a board certified surgeon from the exact same specialty as the defendant provider. The liability chain in an operating room is complex; independent surgeon groups, contracted anesthesia providers, and hospital employed nurses all fall under different corporate entities. Florida has abolished joint and several liability, meaning each defendant pays only their percentage of fault. We identify and name every responsible party during the pre suit period. For the full legal framework including the comparative negligence exemption, the informed consent requirements, and the types of damages available in surgical error cases, see the linked guides.
A surgical error is not a “normal risk.” If you or a loved one has been seriously injured as a result of a surgical mistake in the State of Florida, the experienced Law Offices of Jorge L. Flores, P.A., can help.
From our offices in Miami, Florida, we secure the operative reports, depose the surgical team, retain board certified experts from the exact same specialty as the defendant, and build the comprehensive evidentiary case that Florida’s pre suit requirements demand. We handle surgical malpractice cases on a contingency basis; you pay nothing unless we recover for you.
P.S. The hospital where your surgery took place has already retained legal counsel. Their risk management team has reviewed the operative report, interviewed the surgical staff, and begun constructing a defense designed to characterize your injury as a “known complication.” At the Law Offices of Jorge L. Flores, P.A., we move with the same urgency on your behalf; because the operative records, the anesthesia logs, and the nursing notes that prove exactly what happened in that operating room are the evidence that defense teams work hardest to sanitize.
Related: Medical Malpractice · Complication vs. Negligence · Informed Consent · Medical Records Guide · Who Can Be Held Responsible


